Содержание:
- 1 Introduction
- 2 How does human papillomavirus infection manifest itself in women?
- 3 Why do they appear
- 4 What is the danger of pointed formations?
- 5 Locations (inside, at the entrance) of genital warts and their types
- 6 How infection occurs
- 7 Symptoms of genital warts
- 8 How to diagnose?
- 9 treatment
- 10 Features of treatment in pregnant women
- 11 prevention
- 12 Forecast
- 13 Conclusion
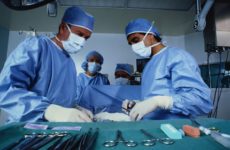
Introduction
Vaginal warts in women are one of the signs of human papillomavirus infection . These are small neoplasms of flesh, pink or brown color.
Without proper treatment, they often cause inconvenience during intercourse, get injured and become inflamed. At the slightest suspicion of warts, you should immediately contact a gynecologist for diagnosis and qualified assistance.

How does human papillomavirus infection manifest itself in women?
Papillomavirus infection is especially dangerous because it can be in the carrier’s body for a long time without showing itself. A person, without knowing it, spreads the pathogen for several months or even years. During an exacerbation, the infection manifests itself in the form of papillary formations on different parts of the body:
- external and internal genital organs;
- in the perineum;
- around the anus;
- in the region of the urethra;
- on the thighs;
- on the neck and eyelids.
The genitals are most often subject to the appearance of warts. Warts cause itching and burning, interfere with wearing underwear, have an unpleasant odor, and lead to the formation of ulcers.
Why do they appear
The only cause of vulvar warts is infection with the human papillomavirus. During the incubation period, it does not cause trouble. A number of factors lead to its activation and, accordingly, the development of genital warts:
- hormonal disruptions, including pregnancy;
- seasonal hypovitaminosis;
- systematic stress and overwork;
- hypothermia;
- weakening of the immune system, for example, due to the use of antibiotics;
- sexually transmitted diseases;
- mucosal injury;
- metabolic disease.
What is the danger of pointed formations?
Genital warts are dangerous because of their location. They are constantly injured during intercourse, hygiene procedures or putting on underwear. Such injuries lead not only to bleeding, but also to infection with various infections that penetrate into the injured areas.
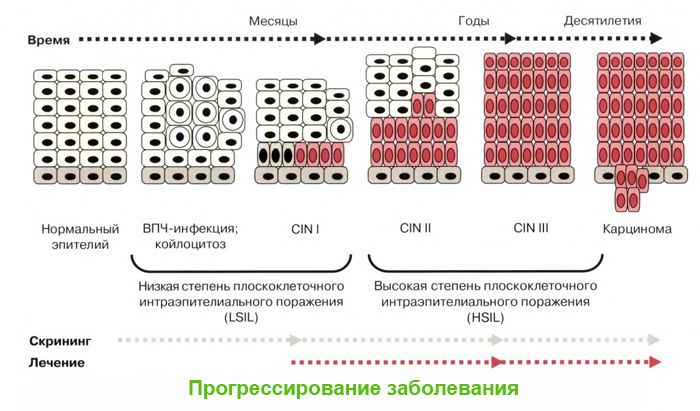
A woman constantly feels physical discomfort, subsequently accompanied by moral. She avoids sexual relations, neglects hygiene, which necessarily affects her mental state. It has been proven that in advanced stages, warts become malignant, that is, they lead to cancer of the female genital organs.
Locations (inside, at the entrance) of genital warts and their types
Neoplasms appear both on the external and internal genital organs. At first they are single, but without treatment they become multiple. Warts form growths resembling cauliflower, noticeably increase in size. According to their form, they are divided into two main types:
- Pointed. Significantly protruding formations with uneven edges. They are localized at the entrance to the uterus, at the anus, near the urethra and on the mucous membrane of the labia.
- flat. Elongated warts of gray or beige color, almost imperceptible. The surface is rough and uneven. They are located on the cervix, causing its erosion, as well as on the walls of the vagina.
How infection occurs
There are three main ways of infection with warts:
- Sexual . The most common, the virus enters the bloodstream through the mucous membrane of the genital organs, especially if they are damaged.
- domestic. Rarely, infection occurs through hygiene items (towel, bar soap, underwear), as the virus can live in secretions.
- From mother to child. Warts can be inherited at birth.
Symptoms of genital warts
It is often possible to determine the presence of warts only on examination by a gynecologist, since they are rarely visible to the naked eye. However, there are several signs of warts on the genitals:
- itching in intimate places ;
- feeling of discomfort, foreign body;
- pain and bleeding during or after intercourse;
- purulent discharge with an unpleasant odor;
- irritation of the vaginal mucosa.
How to diagnose?
To determine the presence of genital warts, you should contact a specialized doctor: a gynecologist or dermatovenereologist. Often, consultation with a therapist, endocrinologist, proctologist is required. Specialists use the following diagnostic methods:
- Anamnesis . Collection of information about heredity, the duration of discomfort and their severity, the characteristics of sexual activity, the presence of concomitant diseases.
- Gynecological examination using a mirror and a colposcope . Allows you to determine the exact number of neoplasms and their location.
- anoscopy . Inspection of the anus to determine the spread of the disease.
- Cytology . Collection of fragments of genital warts to study their nature under a microscope.
- Clinical blood test to determine the presence of sexually transmitted diseases.
- Scraping of epithelial elements and their study for the presence of human papillomavirus. With a positive result, the type, quality and quantity of viral cells are identified.
treatment
The effectiveness of this or that method of treatment depends on the number of condylomas, their location, the degree of growth, the individual tolerance of the selected drugs. Any way to get rid of warts involves the use of vitamin preparations, restorative therapy.

Medical
Small single growths can be removed by conservative methods. The doctor prescribes antibacterial and healing drugs in the form of ointments. A woman can apply them herself at home daily at bedtime for at least 2 weeks. If warts are not located in the field of view, candles, for example, betadine, will be effective.
In order to strengthen the immune system and reduce the activity of the virus, rectal administration of viferon suppositories is prescribed. They are used twice a day for 10 days. It is good to combine them with panavir antiviral injections . It is usually given every 24 hours for 2 days, followed by three more shots every other day.
Under the supervision of a gynecologist, warts that have not had time to grow are removed using local remedies. Most often, these are preparations based on salicylic acid, solcoderm. They are applied pointwise, without affecting healthy tissues. The procedure is repeated several times until the complete death of the condyloma tissue.
Surgical methods
Multiple warts, especially those that cause significant inconvenience, are located deep or tend to become malignant, are removed by one of the surgical methods. The most popular include:
- laser. Removal of affected tissues occurs with a laser knife and under a microscope. The operation is characterized by high precision, after it there are no noticeable scars. Even warts on the cervix can be easily eliminated with a laser. Moreover, the operated site is immediately cauterized, which eliminates bleeding.
- electrocoagulation . The most affordable way, however, requiring a long recovery. Removal of warts occurs with the help of electrical impulses. After the operation, a wound remains, which can be delayed up to 2 weeks. Patients note the pain of this method.
- radiosurgery . To date, the most effective method: the risk of recurrence of genital warts is minimal. In addition, the doctor removes only damaged tissues with a radio wave knife, without touching healthy ones. The advantages of the operation are painlessness and speed. Recovery doesn’t take long.
- Cryodestruction . Genital warts are frozen with liquid nitrogen. The operation is quick and relatively painless, and scars rarely remain after it. Recovery takes 1-1.5 weeks. However, the method has a number of contraindications, for example, the impossibility of treating the cervix due to the fact that the device does not penetrate so deeply. In addition, cryodestruction is not used for those women who plan to give birth. The epithelium after such an intervention loses its elasticity, which negatively affects the reproductive health of a woman.
- traditional . The doctor uses a conventional scalpel to remove the affected tissue. This method is used extremely rarely, only if there are indications, for example, if condylomas have grown to a critical state. The operation is not highly effective due to the duration, pain, and the need for anesthesia. In addition, the doctor is not always able to remove condyloma without involving healthy epithelium. The recovery period may be accompanied by pain and bleeding.
Features of treatment in pregnant women
If warts are found in a pregnant woman, in most cases they must be removed to minimize the risk of infecting the baby. An exception is neoplasms located not in the vagina and on the cervix, but, for example, near the anus.
If warts do not pose a danger to the child, they are recommended not to be touched before childbirth. After them, as a rule, the death of condyloma cells is observed. Otherwise, treatment is prescribed after childbirth and the recovery period.

If condylomas are in the birth canal of a child, they must be disposed of. Usually, at first, doctors recommend traditional methods: they prescribe antiviral drugs and immunomodulators. External condylomas are removed by cauterization with acid-containing agents: duofilm, collomak .
Of the surgical methods, a pregnant woman who has no contraindications may be recommended cryodestruction or a laser method. They do not require the introduction of painkillers and are especially effective in the treatment of the cervix.
prevention
If a person is not infected with papillomavirus infection , then the risk of its occurrence can be reduced with the help of two- and four-valent vaccination and subject to the use of barrier methods of contraception. But even if a woman is already a carrier of the virus, the occurrence of vaginal warts can be prevented by adhering to the following rules:
- proper nutrition;
- rejection of bad habits;
- personal hygiene;
- timely treatment of diseases of the pelvic organs;
- regular examinations (1-2 times a year) at the gynecologist;
- exclusion of casual sexual relations;
- taking vitamins and strengthening the immune system;
- observance of the regime of work and rest, walks in the fresh air.
Forecast
With timely access to a doctor and removal of warts, the prognosis is favorable: the risk of recurrence is minimal. It is impossible to get rid of the causative virus, however, repeated condylomas may occur only after a few years or not appear at all. The main thing is to prevent their growth and malignancy. Otherwise, the likelihood of cancer of the genitourinary organs is high.
No doctor will undertake to accurately predict whether neoplasms will occur. But all of them will unanimously recommend monitoring the state of the immune system. The slightest failure in its work leads to an exacerbation of a viral infection living in the body.
Conclusion
Genital warts are not a sentence, in many cases they are amenable to conservative treatment. And thanks to modern surgical methods, the affected tissue can be removed quickly and painlessly. By adhering to complex antiviral therapy and simple preventive measures, it will be possible to reduce the risk of recurrence of growths.